|
4/12/2024 0 Comments Medicare abcd explainedAdditionally, each plan has a coverage gap (also called the “donut hole”). Deductibles, copayments, and coinsurance rates vary plan to plan within certain limits set by medicare. Premiums vary according to the plan selected as well as the income of the beneficiary. These plans have premiums that are in addition to the medicare part B premium. Medicare Part D: Various commercial health companies offer Medicare prescription drug coverage plans. Home health care has no deductible or co-insurance payments.įor Part B, the beneficiary pays one annual deductible of $198, the monthly premiums, and co-insurance payments of 20% of the medically allowed charges. Medicare payments stop after 90 in-patient days, unless the beneficiary elects to use "lifetime reserve" for which a co-payment of $704 per day is required.įor skilled nursing care, the first 20 days are fully covered, but days 21 through 100 require a co-payment of $176 per day. If continued care is needed beyond 60 days, (days 61-90) additional co-insurance payments of $352 per day are required through hospital day 90. This covers the beneficiary's first 60 days of each period of hospital care. Plans may have additional costs as well as provider and coverage limitations.įor Part A (hospital insurance), the beneficiary's payment share is a one time deductible of $1,408 at the beginning of each benefit period. Many plans offer extra coverage such as dental, hearing, vision, and prescription drug coverage. If a Medicare beneficiary joins a Medicare advantage plan, the plan provides part A (hospital insurance) and part B (medical insurance). These policies must meet Federally imposed standards, and are offered by commercial health insurance companies, such as Blue Cross and Blue Shield. 
These plans are also called Medicare Advantage Plans or Medicare Part C. Medigap refers to private insurance policies that will pay most of the health care charges not covered by Parts A or B. These liabilities may be paid "out of pocket" by the beneficiary, or by a third party insurance company as part of a "medigap" coverage plan. The premium is usually deducted from the Social Security benefit checks of those enrolled in Part B.īeneficiary Payment Liabilities and Medicare Part C: Beneficiaries are responsible for charges not covered by the Medicare Program and for the various cost-sharing aspects of Parts A and B. In 2020, the standard part B premium was $144.60 per month, but this amount increases for individuals with incomes >$87,000 per year. Medicare Part B Financing: Medicare Part B is financed through general federal revenues (72%), premiums (26%), and interest and other sources (2%). The hospital insurance funds can be used only to pay for the Medicare Part A, and Part B funds cannot be transferred for Part A use. The taxes paid each year are used primarily to pay benefits for current beneficiaries. The trust fund also receives income from a portion of income taxes levied on Social Security benefits paid to high income beneficiaries, premiums from those who are not otherwise entitled Medicare benefits and choose to enroll voluntarily, and interest earnings. 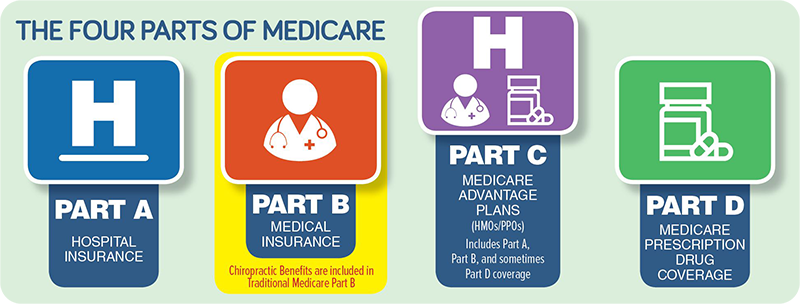
The money is paid into a trust fund that is a special account in the U.S. Medicare Part A Financing: Financing for the Hospital Insurance Program is primarily through a mandatory payroll deduction, the "FICA tax." Currently, the FICA tax is 1.45% of earnings paid by each employee and their employer, or 2.90% for the self-employed.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
